
Long Island Asthma Doctor
Seeking expert asthma care in the Long Island area? Our Long Island Asthma Doctor is here to provide top-notch, specialized care for asthma patients. With a profound understanding of asthma management and treatment, our Long Island-based asthma specialist offers comprehensive diagnostic and therapeutic services tailored to meet the unique needs of each patient. From thorough lung function testing to personalized treatment plans, our Long Island Asthma Doctor is dedicated to helping you breathe easier and improve your quality of life. Whether you’re dealing with mild intermittent asthma or more severe forms, trust our skilled asthma doctor in Long Island to deliver exceptional care and support every step of the way.
36 Years of Experience
Accepts Most Health Insurances
Award-Winning & Recognized Medical Leader
Board Certified Allergist & Immunologist
Asthma offices in Massapequa, Plainview, North Babylon, Coram.
Top-Rated Allergist & Immunologist In New York
Asthma Specialists
The allergy, asthma, and immunology team of Heart & Health diagnose, treat, and manage immunologic conditions including allergies, asthma, autoimmune diseases, autoinflammatory syndromes, and immunological deficiency syndromes. Led by renowned Allergist Dr. Louis E. Guida, Jr., the team at Heart and Health Medical is comprised of board-certified Allergists and Immunology specialists and equipped with the most advanced equipment and facilities in Long Island, New York with four locations in Massapequa, Coram, North Babylon, and Plainview.
Patient Reviews
Louis E Guida, Jr. MD, FCCP, FAAAAI, FACAAI
Board Certified in Allergy, Asthma and Immunology, Pediatrics
Dr. Louis E. Guida Jr. is a renowned Allergy & Immunologist with over 36 years of experience diagnosing, treating, and managing allergies, asthma, and immune disorders for members of the communities of Long Island, New York. Dr. Guida was initially awarded his medical degree from St. George’s University School of Medicine. He completed his internship and residency in Pediatrics at Monmouth Medical Center, Long Branch, New Jersey. He went on to complete two fellowships – Cystic Fibrosis (Adult and Pediatric) and Pediatric Pulmonology at Hahnemann University Hospital in Philadelphia, Pennsylvania, and Adult & Pediatric Allergy / Immunology at Nassau County Medical Center in East Meadow, New York.
Dr. Guida’s hospital affiliations are Good Samaritan Hospital Medical Center in West Islip, New York, and St. Charles Hospital, Port Jefferson, New York. He is an adjunct clinical assistant Professor of Pediatrics at the New York College of Osteopathic Medicine. He is the Medical Director of the adult and pediatric Cystic Fibrosis Programs and the Family Asthma and Allergy Center at Good Samaritan Hospital Medical Center. He is a fellow of the American Academy of Allergy, Asthma and Immunology, American College of Chest Physicians, and the American Academy of Pediatrics.
Specialties
- Adult & Pediatric Asthma
- Allergy
- Pulmonology
Hospital Affiliations
- Good Samaritan Hospital Medical Center
- St. Charles Hospital
Fellowships & Memberships
- Fellow of The American Academy of Allergy, Asthma and Immunology
- Fellow of The American Academy of Pediatrics
- Fellow of The American College of Allergy, Asthma, and Immunology
- Fellow of the American College of Chest Physicians
- New York Allergy Society
- Long Island Allergy Asthma Society
- Cystic Fibrosis Foundation
- American Medical Association
Accepted Insurances





















Asthma Symptoms, Diagnosis, and Treatment
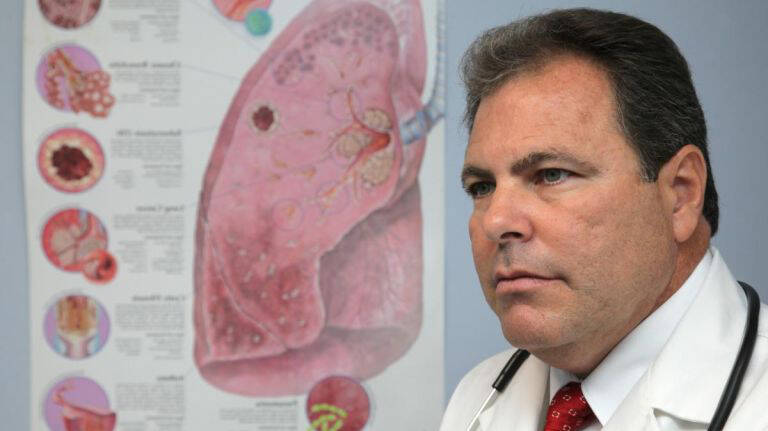
What is Asthma?
Asthma is a chronic respiratory condition where the airways in the lungs become narrowed and inflamed, often producing extra mucus. This can lead to breathing difficulties, coughing, wheezing when exhaling, and shortness of breath. Asthma’s impact can range from a minor annoyance to a severe disruption of daily life, and in some cases, it can lead to life-threatening attacks.
Types of Asthma Based on Severity:
Mild Intermittent Asthma: Symptoms less than twice a week; nighttime symptoms less than two times a month. Lung function tests show 80% or more of predicted values. No long-term medications required.
Mild Persistent Asthma: Symptoms three to six times a week; nighttime symptoms three to four times a month. Lung function tests show 80% or more of predicted values.
Moderate Persistent Asthma: Daily symptoms; nighttime symptoms five or more times a month. Lung function tests show 60%-80% of normal values.
Severe Persistent Asthma: Continuous symptoms with frequent nighttime asthma; significant activity limitation. Lung function tests show less than 60% of predicted values.
Asthma Symptoms:
Asthma symptoms can vary widely among individuals. Common signs include:
- Shortness of breath.
- Chest tightness or pain.
- Wheezing when exhaling, particularly in children.
- Difficulty sleeping due to breathing problems.
- Coughing or wheezing attacks worsened by respiratory viruses.
Diagnosing Asthma:
Diagnosis involves:
- Taking a medical history and observing breathing.
- Performing lung function tests, such as spirometry, to measure air exhalation.
- Possibly conducting a methacholine challenge test if initial tests are inconclusive. A positive test indicates asthma if lung function drops by at least 20%.
Asthma Treatment:
Asthma management includes using prescribed medications, avoiding triggers, and monitoring symptoms. The main types of asthma medications are:
Anti-inflammatories: Essential for most people with asthma, these medications, like inhaled steroids, reduce airway swelling and mucus. They require consistent daily use and may take weeks to control asthma.
Bronchodilators: These relax the muscles around the airways, improving airflow. They come in short-acting and long-acting forms and can also be used for exercise-induced asthma symptoms.
Proper medication adherence, along with lifestyle adjustments and regular medical consultations, is key to controlling asthma and maintaining quality of life.
Hospital Affiliations





Find An Asthma Doctor Near You
Coram: 3650 Route 112, Coram, NY 11727
Levittown: 1 Center Lane, Levittown 11756
Massapequa: 6175 Sunrise Highway, Massapequa, NY 11758
North Babylon: 1350 Deer Park Avenue, North Babylon, NY 11703
Plainview: 1070 Old Country Road, Plainview NY 11803
